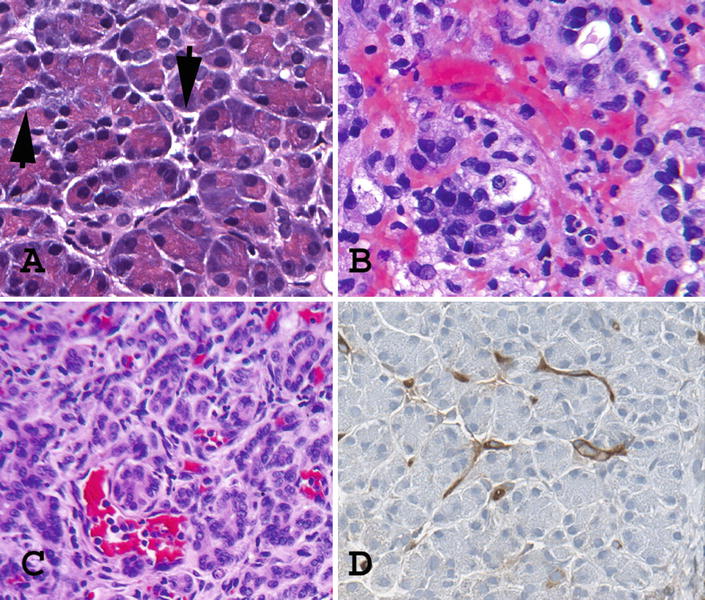
Rejection Of The Transplanted Pancreas
 What is rejection ?
What is rejection ?
The immune system in the human body cannot distinguish between the transplanted pancreas and the unwanted invaders, such as viruses and bacteria. So, when a pancreas is transplanted from one person (the donor) into another (the recipient), the immune system of the recipient triggers the same response against the new organ that it would have against any other foreign material, thus setting off a chain of events that can damage the transplanted pancreas. This process is called rejection. It can occur on the operation table (Hyperacute rejection), rapidly (Acute rejection), or over a long period of time (Chronic rejection). Rejection can occur despite close matching and HLA typing between the donor and the transplant recipient.
 How is rejection prevented ?
How is rejection prevented ?
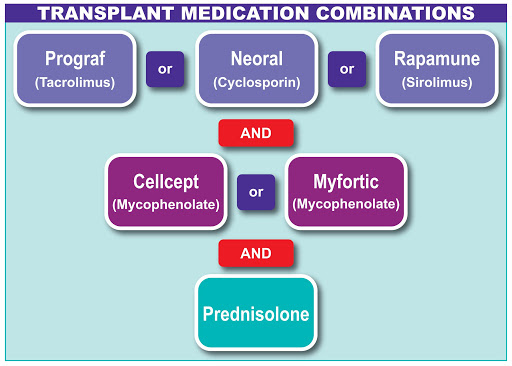
After any pancreas transplant, patient will receive special medications called immunosuppressants. These are the drugs that weaken the immune system's ability to reject newly transplanted pancreas. This greatly decreases the risks of rejection, protecting the new organ and preserving its function. However, this may put the recipient at greater risk of infections, mostly for the first 3-6 months after transplant. A wide variety of these drugs are available with differing mechanisms of action. This include Alemtuzumab (given at the time of surgery and for one day afterward) and Steroids, Cyclosporine, Tacrolimus, Sirolimus or Mycophenolate mofetil (given for long term therapy). One or more of these drugs must be taken exactly as prescribed by your transplant team for the rest of your life.
 How is rejection treated ?
How is rejection treated ?
Most of the rejection episodes can be treated medically. The earlier the rejection is diagnosed, the more successful the treatment is likely to be. That’s the reason it is important to be in regular follow-up with your transplant team.